John Tolley, September 19, 2016
The Challenge
Diabetes, the family of metabolic disorders characterized by elevated levels of blood sugar, can give rise to a whole host of nasty effects including heart disease, kidney failure, and elevated risk of stroke. Yet one of the most insidious risks comes from something seemingly benign.
Diabetic foot ulcers occur in 15 percent of diabetes cases. Small injuries to the foot, which in most people would heal naturally, remain in a perpetual state of inflammation due to the nature of the disease.
?Too much glucose, or sugar, in the bloodstream can cause nerve damage and microvascular circulation problems,? explains Yunxiao Zhu, a doctoral student at Northwestern University. ?When wounds arise, they are very hard to heal and highly easy to get further contaminated by bacterial infections.?
If left untreated, diabetic foot ulcers can lead to necrosis which can result in amputation of the foot or entire lower leg.
The Idea
Zhu and a team of researchers led by Dr. Guillermo Ameer at Northwestern have developed an innovative type of bandage that treats the very specific problems surrounding diabetic foot ulcers.
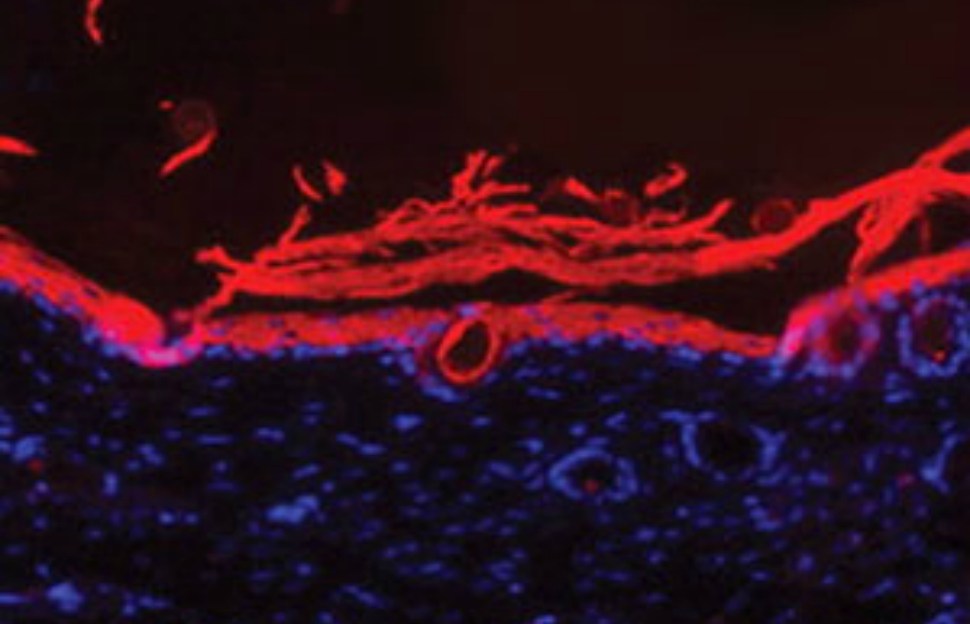
Consisting of an antioxidant hydrogel, the bandage?s thermo-responsive nature causes it to stiffen upon contact with the body. The material reduces oxidative damage and keeps the wound moist while releasing the highly potent chemokine SDF1, a protein that speeds healing by promoting micro blood vessel formation.
?One of the reasons diabetic wounds are hard to heal is due to impaired microvascular circulation,? says Zhu, first author on the team?s research paper published in the Journal of Controlled Release. ?By restoring the circulation, our bandage has been shown to improve the healing speed of these nasty wounds.?
The team at the Ameer Research Lab has been working on this treatment method for four years, envisioning the bandage as an ideal bio-scaffold for the tissue regeneration needed to needed to heal diabetic foot ulcers.
The Next Steps
Zhu and her colleagues are now undertaking small animal testing with the bandage. If all goes well, they?ll move on to trials with larger animals. Additionally, Zhu is working on other applications for the hydrogel.
?The material is intended for all kinds of tissue-engineering applications,? notes Zhu. ?I?m currently working on using this material as [a] scaffold for pancreatic islets transplantation.?
Zhu, whose undergraduate degree is in pharmaceutical science, says she was drawn to Northwestern for the opportunity to do extensive application-based research with the Ameer Lab. And the chance to work in concert with multiple departments has added a meaningful dimension to her endeavors.
?[I] love the way we can collaborate with the people within the biomedical engineering department and from the medical school so easily,? Zhu explains. ?It really helps to get inspiration and get the sense [of] what kind of technology is actually needed to help patients.?
(Image courtesy of Northwestern McCormick School of Engineering)